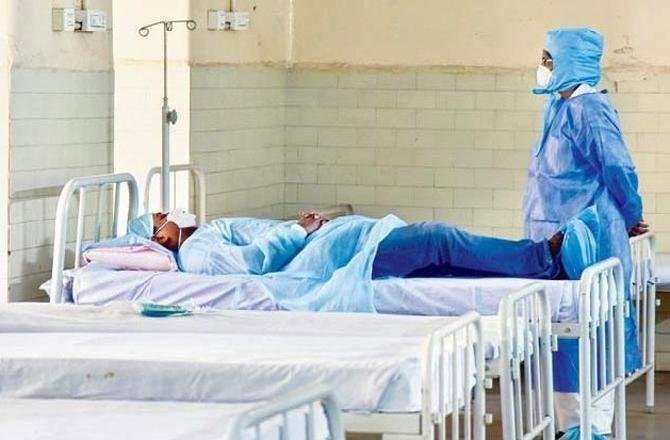
After a brief surgical hiatus, a neurosurgeon walks into a COVID-19 battleground to experience the most impersonal but moving procedure of his life.
We need to do a tracheostomy on a COVID patient,” came the call from the ICU; the first thing I heard when I answered. No formalities or niceties exchanged; this was purely medical talk. A tracheostomy is a surgical procedure that involves making a small cut over the neck just below the Adam’s apple, followed by a tiny hole in the windpipe, in order to place a breathing tube. This is performed in patients infected with the Coronavirus, who’ve been connected to a ventilator but are unable to come off it. A tracheostomy bypasses the nasal passage, reducing airway resistance and hence the effort required to breath, enabling a possibly faster weaning off from the ventilator.
This procedure is generally performed by ENT or head and neck surgeons. The ones affiliated with our hospital had certain health and age issues, making it risky for them to work in a COVID-19-infused environment, especially as this is a high-risk aerosol-generating procedure, which has a lofty chance of exposing healthcare workers to the virus. As neurosurgeons, we routinely perform tracheostomies in patients with head injuries who we suspect will need prolonged ventilation; hence, this is part of our training, and a few hundred cases later, expertise.
“I’ll be there,” I replied after a pause, without asking any questions. The clamour in the background made me aware that the ICU was busier than usual, and that it wasn’t the time to make small talk. Our hospital has temporarily been converted into a COVID-19 unit and is doing a remarkable job saving lives that were nearly lost on the way to the hospital. Getting dressed to work in a COVID-19 ICU requires regimental ferocity: we put on a pair of gloves, a cap, an N95 mask, another surgical mask over it, a full white body suit, goggles, head gear that made me look like a pharaoh, a face shield, and another pair of gloves. The only part of me that was visible were my pupils (if they hadn’t been obscured by the fogging of the glasses due to heavy breathing). You need to walk gingerly, taking small steps lest you trip over something that isn’t visible to you. People identify you by the name scribbled over your suit, and once you start going daily and the nurses like you, you might get an extra heart or smiley face drawn for you next to your name.
The ICU looks more like a NASA space station playing Pac-Man: everyone is either walking towards or away from you. You need to raise your voice to be heard through three layers covering your mouth and across two layers into someone’s ear. Even with this much protection, we continue to maintain physical distance. The virus has annihilated hundreds of years of the caste system; we are all untouchables now.
A colleague positioned the patient with his neck extended. The anaesthetist stood at the head end, ready to withdraw the existing tube. The patient was given a muscle relaxant to ensure he didn’t move or, more importantly, cough, engulfing us in a cyclone of the virus. We cleaned the neck with a greasy pink solution to render it sterile and covered the area around with green drapes. All the instruments were neatly arranged on a makeshift trolley.
Before I started, I put on a surgical gown and my third pair of gloves. I palpated the cricoid cartilage and suprasternal notch with my index and middle finger and made a sharp clean cut between the two. I briskly dissected the layers, working a pair of blunt forceps in repetitive movements until I reached the glistening tracheal rings. I rubbed against them to remove the surrounding tissue. In several COVID-19 cases, I’ve noticed that the trachea is more friable than its usual firm self—perhaps an effect of the atrocity of the germ on the airway.
Once the stage was set, the next one minute was an orchestrated symphony. We stopped the ventilator and cut a small square in the trachea. We held our collective breath; pausing the ventilator to avoid a blast of air hitting us, and holding our breath to prevent us from inhaling it if it does. I took hold of the trach tube, while the anaesthetist withdrew the original tube, and in a swift motion, placed it into the opening. We then removed the retractors and inflated the cuff of the trach tube with all eyes on the monitor to ensure that oxygen saturation didn’t drop. The trach tube was then connected to the ventilator and we watched for chest expansion, which tells us that our tube is in place. Further confirmation was provided by square waves on the monitor and numbers that flutter close to 100.
I made a stitch to tighten the incision and a took a tie to secure the tube around the neck. While we were cleaning up, I checked on how everyone was doing in general, making sure their families were safe; there is always a lurking fear in all of us that we may infect an elderly parent or a little one bouncing in our arms once we return home from such a surgery.
In his remarkable biography of cancer, The Emperor of All Maladies, Siddhartha Mukherjee elucidates, “When a disease insinuates itself so potently into the imagination of an era, it is often because it impinges on an anxiety latent within that imagination.” It is probably exactly the same with this virus. I am now directed to a cordoned-off area in the ICU where I doff my armour, a process that takes close to 30 minutes. I peer at the imprint of a tightly fitted mask on the skin of my face, a testament to having returned from war. I wash my hands, head, and neck along with my spectacles, letting the soap lather well beyond the stipulated time and repeat it thrice, knowing fully well I may have to be back the next day, repeating the entire cycle for another patient.
It is unfortunate but there is something deeply impersonal about operating in this unforeseen and unconventional environment. I don’t know who the patient is. I haven’t spoken to the family; it’s been done by the ICU team over an iPad to minimise contact. I’m just a technician here, placing a tube into a pipe. When we operated in saner times, I knew every detail about my patient and the families: what they did for a living, what their hobbies were, what bothered them, and what ached them beyond their illness. We sat with pain and joy together. This is no more the case. Making a hole in someone’s trachea leaves me with a small hole in my heart. I guess you cannot walk out of battle unscathed, even if you win.
“Why are doctors and health care workers making such a big deal about this war against the Coronavirus?” a friend recently asked me. “Isn’t it the same as what our soldiers at the border do? It’s your duty!”
“It’s probably similar,” I said, “The only difference is that here, we are taking our families to war with us.”