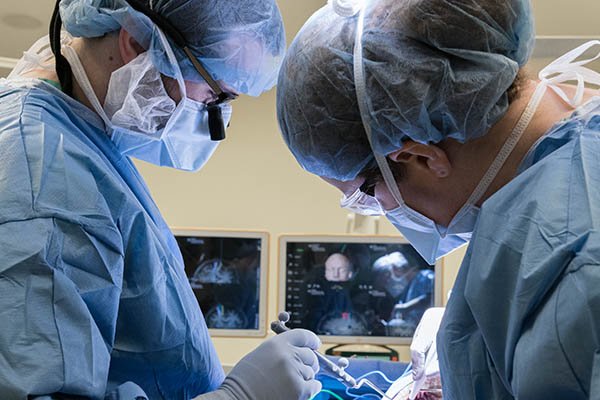
As neurosurgery takes a seasoned cast and crew. And a ceremony marked by detail and diligence
When a friend inquired who would operate on a common buddy’s spinal cord tumour, I said, “Of course, me!” He was only expressing the confusion most regulars experience when a loved one is wheeled into the operating theatre (OT).
I realised, not everyone knows what goes on inside.
So, here’s a little peep.
A patient is usually wheeled into the bay area of the OT early morning. This is where the ward nurses transfer information to the OT nurses, offering details about the patient’s identity, hospital ID, allergies, etc. Meanwhile, the anaesthesiologists chat up the patient to make sure all investigations are in order, check vital parameters. And off the patient goes into the main OT.
The room is usually freezing at 16 degrees, and patients are offered a warm blanket. They lie on their backs staring at the ceiling while the staff goes about its business. Some go silent and quietly follow instructions. But, I’ve also had patients who weep or laugh uncontrollably.
Meanwhile, the scrub nurse prepares a trolley decorated with instruments. The circulating nurse is a goafer available for last-minute requirements, handing them over to the scrub nurse who is sterile (not physiologically, of course).
The anaesthetists simultaneously prepare their trolley, loading up medication as the OT technician sets the operating table for height and function. The anaesthetists fix and secure an intravenous and intra-arterial access after hooking up the patient to the various ECG leads. We usually say, “Sweet dreams!” to the patient before they are given a cocktail of the ‘happy stuff’ that knocks them out. The breathing tube is inserted and the patie nt is connected to a ventilator. While this is being done, the neurophysiologists connect their electrodes to monitor the motor and sensory function of the patient under anaesthesia, in case we need to operate close to vital structures.
nt is connected to a ventilator. While this is being done, the neurophysiologists connect their electrodes to monitor the motor and sensory function of the patient under anaesthesia, in case we need to operate close to vital structures.
When I’m operating on the brain, I check for the side I need to operate on more than once before I mark the incision spot on the head. An operation on the spine requires a cut down the centre; otherwise, I’m paranoid about operating on the wrong side. Cardiac surgeons are eternally grateful that they never have to face this problem.
Another nurse inserts a urinary catheter, and once the patient is ready to be positioned, at the count of three, we turn the patient on the back in one swift move. Respective teams recheck if all paraphernalia is still connected, the position is optimal and the knees and elbows are padded to prevent undue pressure. The X-ray machine is brought in to confirm and mark the desired level we plan to open up to.
Then, the circulating nurse calls for a ‘time out’. Everyone stops what they are doing. As funny as it sounds, we check once again that this is the same patient we need to operate on and that the hospital ID matches.
“Name of the procedure?” the lead nurse calls out clearly, silencing everyone in the room as she goes through her step-wise checklist. “D10-12 laminectomy and excision of intramedullary spinal cord tumour,” I say.
“Sterility confirmed?”
“Yes,” says the scrub nurse.
“Any equipment issues?”
“No,” she says.
“Not yet!” I interject, knowing that something might need reworking.
“Antibiotics administered?”
“Yes,” say the anaesthetists.
“Anticipated blood loss?”
“200 ml,” I say. This is usually followed by a smile from the anaesthetist. Surgeons constantly underestimate the amount of blood they will lose in an operation; it’s an
ego issue. Anaesthetists are overcautious about ensuring that adequate blood is arranged for; it’s a safety issue. And this is reason for friendly banter.
“Okay, you can proceed,” is the close of the circulating nurse’s checklist.
We scrub the back with three solutions for 10 minutes, while one of us gets ‘washed up’ and ready to place sterile drapes on the patient. There is usually a primary surgeon who performs the operation, while an assistant surgeon helps. Depending on the ease of the procedure, we swap steps if we are training a colleague or perform tasks simultaneously to speed things up. The mood and tone of the conversation during surgery varies with the complexity of the procedure, the quality of the scrub nurse, how well the surgeon and anaesthetists get along, and so on. Once we are done, we place a dressing over the wound, carefully flip the patient back, and prepare to remove the breathing tube.
Once the patient is partially awake, we check to see if they are able to move their arms and legs adequately. I usually leave the OT with, “Thank you, everybody” and head out to talk to the family, while the patient gets cleaned and mobilised to the recovery area.
This is how we do it, every day, sometimes three times a day. Each day brings with it another patient, another family, and another chance to make a difference to a life.