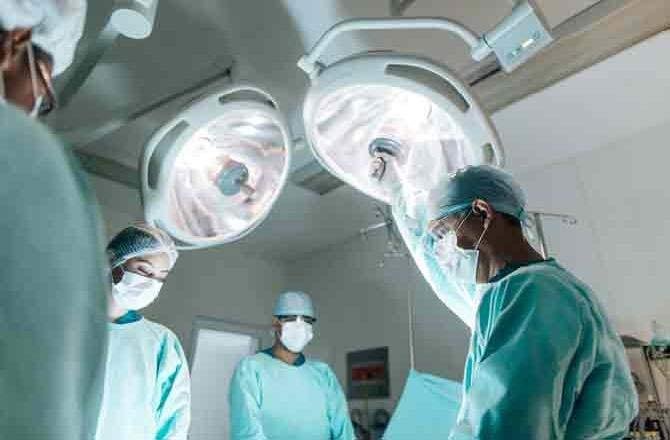
I plugged in the cerebral angiogram films against the white light of the view box and explained the imaging findings to Ryan. Ryan was a handsome, 38-year-old software engineer.
He wore rimless glasses, dark washed jeans, and clean dress shoes—a minimalist look that typified his profession. He had recurring headaches that did not seem to get better with ‘regular’ medication. His family physician had ordered a scan. The brain MRI showed a 5.5 cm tumour arising from the meninges, the protective tissue covering the brain, pressing down on it.